It is projected that within the EU, the percentage of the population over 65 will increase by 80.5% between 2008-2060. Rapid transformations like these within our socio-economic landscape are having profound ramifications for health care systems. There is a growing concern, even in more affluent countries, over how our existing health frameworks will handle an ageing population and the resultant rise in chronic disease and comorbidity.

We are seeing elderly people become dependent not only on their GP but multiple specialists, often travelling to different centres and grappling with misaligned processes in order to access treatment. This is further complicated when patients rely on a mixture of private care, community resources and family support.
Increasingly, the health community is recognising that designing the solutions for this require the patient to be at the centre of the process, and that tech developments will be the linchpin of the preventive, predictive and collaborative treatments necessary to overcome the fractures of our current systems. Around the world there is agreement that health care is at least a decade behind other industries in the use of information technology. It may be even further behind in realising the productivity and value improvements that have been seen elsewhere as the result of information technology.
Around the world there is agreement that health care is at least a decade behind other industries in the use of information technology. It may be even further behind in realising the productivity and value improvements that have been seen elsewhere as the result of information technology.
The State of Play in Digital Healthcare
With big tech working on the future of wearables and start-ups continuing to populate the app stores with resources to aid self-care, there is already clear movement towards more connected healthcare in the future. We still lack, however, a holistic outlook that can scale up to the immensity of the challenge that will be staying healthy in a world that is ever more densely populated and older. This requires bringing the disruptive technologies and design practices currently concentrated in the private sector, into our public health services where there is a much higher barrier to adoption – primarily due to security concerns, budgeting restraints and complicated bureaucracies.
Despite these challenges, the conceptual boundary between ‘health’ and ‘digital health’ is dissolving and there are huge opportunities to address them from a number of perspectives:
- Quality and timeliness of interventions (diagnosis and treatment)
- Accessibility
- Data and measurability
- Cost effectiveness
The potential for each of these areas is galvanising creative output at all intersections of health care – ageing is by no means the only issue that would benefit from more collaborative, multidisciplinary efforts.
The best way to put people at the centre of new healthcare solutions is, we believe, through convening true partnerships between digital health innovators and healthcare experts. Bringing product design skills is not enough – the delivery of person-centred care depends upon our ability to create bridges between institutions, businesses and designers.
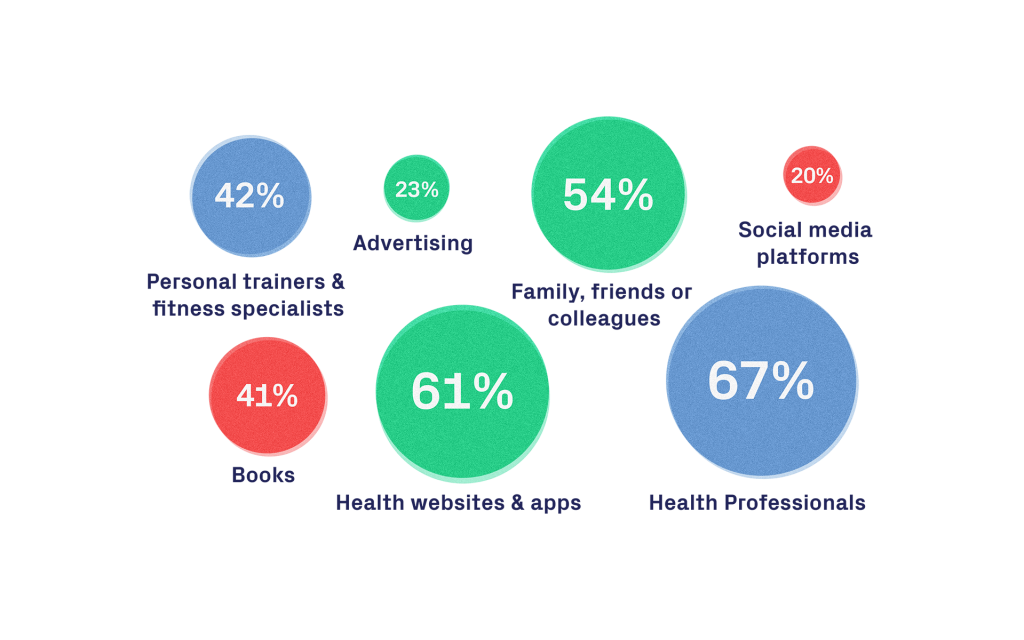
As consumers and patients, we increasingly look for and welcome the insights that digital tools can provide. While healthcare professionals still lead the way, with 67% of people seeing them as their most trusted source for advice about healthy living, they are closely followed by 61% of people who place their trust in health websites and apps to the same degree.3 Using tools online or standalone apps is rapidly becoming an accepted part of an individual’s efforts to stay healthy.

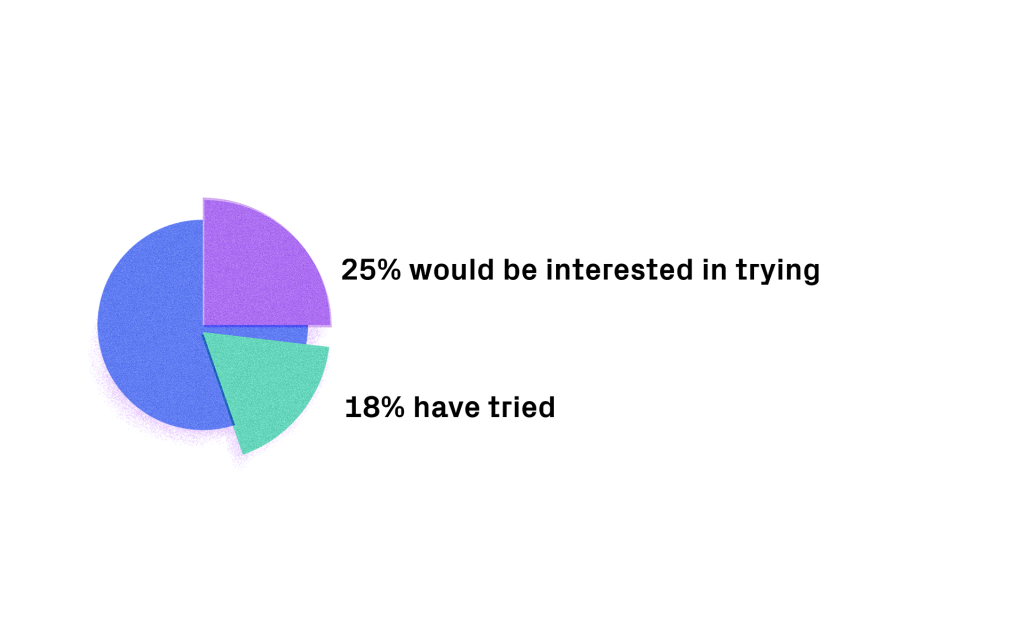
In the UK, tracking food or exercise with an app has been tried by 18% of the population, with 25% interested in trying it in the future.4 Adoption of tools like these demonstrates appetite for more autonomous, personalised and precise care, but such applications can lack the scientific rigour needed to make long-term, tangible effects on the user's health. This is no space for complacency – these signs of popular uptake should be a beacon call for innovators to make substantial digital solutions, rather than disposable applications.
Moving Digital Health Forward, Together
It is an area that presents both huge opportunity and serious responsibility alike. As a digital product studio, we have picked our way over this notoriously uncertain ground by drawing on diverse channels of experience. What we bring to partnerships in the digital health space comes from experience of not only working to client briefs but also developing our own products and businesses.
Equally, our ability to develop tools to tackle problems in this space has only been made possible through our working partnerships. In providing an intellectual and methodological counterweight, these relationships will continue to be instrumental in developing much-needed services. Together, with a clear-eyed understanding of each other’s strengths, we can create the right responses.
For us, collaboration is more than shorthand for ‘joint stakeholders’. It means a no-holds-barred relationship, without a strict division of responsibilities. It’s about sharing different perspectives on problem-solving, design, copy, development, features and marketing. It’s about creating a partnership of trust and compromise, where you learn from each other’s skills and expertise to create products that solve problems.
This sort of open and committed collaboration is hard won. For ustwo, it has required finding the right partners who are excited about new processes and, in turn, listening to their expertise just as they listen to ours. This cross-pollination of ideas is key – we encourage our partners to give insight into process and we aim to bring fresh eyes to established ways of working.
Many of our insights into how we build these relationships, and how fruitful they can be, came out of our work on Moodnotes, an app that helps individuals manage their mental health.
Before we began working together, Thriveport’s founders Dr. Drew Erhardt and Dr. Edrick Dorian had already starting working on the interface between mental health and digital solutions with the creation of the app MoodKit. When it came to building Moodnotes, they were able to bring both this experience as well as their years of research, teaching, and clinical work as practicing clinical psychologists specializing in cognitive behavior therapy (CBT) to help improve people’s mental health and wellbeing.
With this key part of the puzzle in place, ustwo were able to add their human-centered design expertise. As a tool that addresses hugely personal often internalised problems, we recognised that user testing at scale was going to be key for validating anything we created. We engaged social media networks to create a trial group with 500 testers. Even from this initial step we garnered affirmation, one-third of the people who saw the landing page went on the sign up for the trial – the demand was out there.
Our relationship with Thriveport continues to sustain our efforts to update and maintain the Moodnotes platform so that it addresses all of our users’ needs. With them to steer the way in terms of content, we have been able to interpret user insight with consistent consideration of the medical implications. At the same time we have continued to amplify the voices of our users by feeding back their requests, compliments and criticism back into the product.
Embedded content: https://vimeo.com/133774167
Staged iterations were also the foundations of PAUSE – a mobile mindfulness and meditation experience developed in Malmö by ustwo Nordics. The initial tests were conducted on participants wearing a Muse brain sensor headband, trying out different concepts for 10 minutes and following up with interviews. Through this early testing we were able to dismiss many other ideas of how to manifest our larger vision of using mobile technology as tool for calming the mind rather than distracting it. The result is the dynamic shape you see on screen today.
To further evaluate PAUSE’s ability to calm the active mind, we sought to build on our user-testing by also turning to scientific specialists for validation. First, We conducted a study using an Emotiv wireless headset to measure EEG-signals. To validate the data from these sessions, we collaborated with Dr. Chi Thanh Vi, Research Fellow in Multisensory Experiences at the University of Sussex. Chi Thanh Vi is an expert in using brain sensing methods to understand the neural basis of different user states when using interactive products. With his analysis, we could interpret the data and show that PAUSE helps to produce a calmer state of mind and a lower mental workload.

A Connected Vision For Healthcare
We are the first to admit that iterating user-feedback and professional validation into healthcare designs is not the same as bringing the human into healthcare. This is something that needs a genuine mindset shift – people need to be able to see products like Moodnotes and PAUSE, electronic health records, the use of wearables for remote monitoring, confidence in secure data and increased patient engagement as compatible solutions to shared problems.
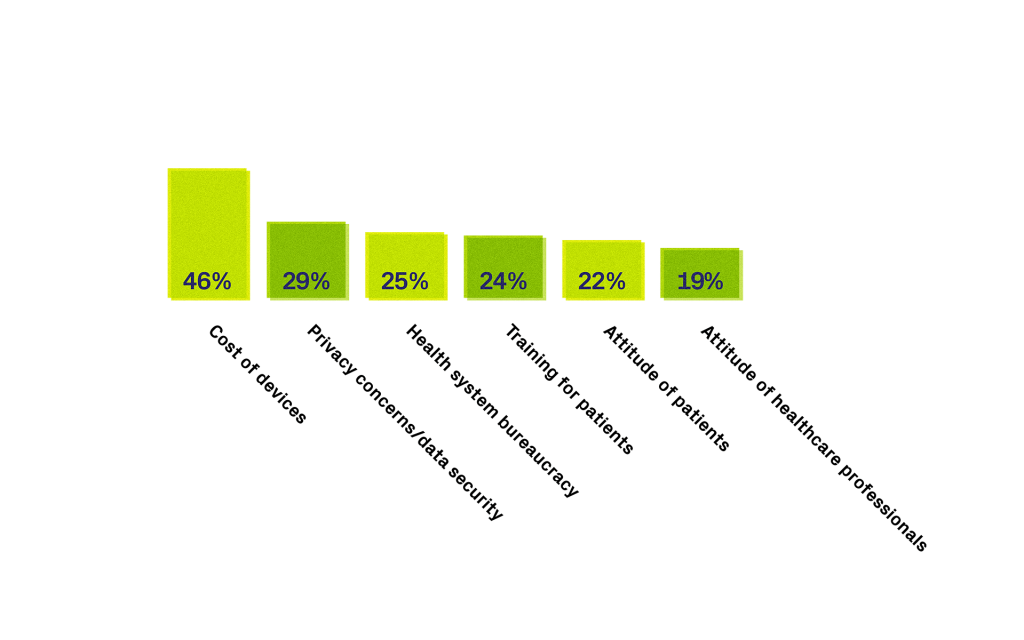
Both patients and healthcare professionals struggle with antiquated systems and struggle with legitimate concerns about how they might be updated. A major concern for HCP in the adoption of new technologies, is the cost of the devices needed to support them. From a patient perspective, those from lower socio-economic backgrounds are more likely to find accessing technology a barrier to treatment.
Digital alternatives also have the power to democratise care and by tapping into technology already accessible to patients and providers, we can help them both save money and get better treatment in the long term. 82% of Brits own a smartphone and tablet saturation is still increasing, as is the proliferation of wearable technology.5 For healthcare providers, this technology is also being seen as essential – Frost & Sullivan cite that “the vast majority of agencies say their employees rely on smartphones, tablets, and even wearable devices to get their jobs done.”6
Embedded content: https://vimeo.com/178460642
In early 2015 ustwo met with City University in London, who were been developing a natural language recognition tool to identify trigger phrases in a carer’s notes and prompt further action. The aim was to merge together City University’s knowledge and technology with the practical, everyday requirements of being a carer.
Keepsake offers the possibility of vast reductions in note-taking, faster referral times to the GP, and sending much-valued information to relatives. It offers a chance to start re-thinking how dementia care happens and, longer-term, how patients and families can interact with their records. It simply could not have happened without collaborative working, both in terms of user testing and with City University.
In this instance, more accurate and personalised notetaking – enabled through technology – gives carers access to more data and allow monitoring in day to day lives. This information will be foundational in deploying targeted treatment that prevents relapse and provides intervention on an individual level.
Our experience with Moodnotes, PAUSE and Keepsake have only made clearer the role that digital design practice can play in bridging the gap between healthcare professionals, patients, and disruptive companies. Together we can scale this work to revolutionise the provision of health care so as to deliver better outcomes to more people with greater efficiency.
There are numerous barriers to progress, but cost and efficacy are by far the biggest. We believe that these issues can be addressed using iterative design, conducted in partnership with domain experts. By researching, understanding and building for the opportunities at all levels of healthcare provision – from the family, to the local, to the national – means creating efficiencies of time, saving unnecessary spend and improving outcomes. These will be the acid-test for the future’s truly useful solutions.
To discuss how ustwo can partner with you on healthcare solutions, get in touch – health@ustwo.com
_Illustrations by Simon Child.
2 A Gaw, Perspectives on Public Health, March 2016
4 Mintel, Healthy Lifestyles - UK - October 2016, Health Information – Who do People Trust?
5 Mintel, Healthy Lifestyles - UK - October 2016
6 Mintel, Digital Trends - UK - Summer 2016
7 Frost & Sullivan, Navigating Digital Transformation in Healthcare, September 2016
